Electrophysiology: How Heart Rhythm Specialists Treat Atrial Fibrillation
Atrial fibrillation, often called AFib, can feel unsettling because it affects the heart’s rhythm — the very timing system that keeps the heartbeat steady and coordinated. Some patients feel fluttering, racing, pounding, skipped beats, shortness of breath, fatigue, dizziness, or reduced exercise tolerance. Others have very few symptoms and only discover AFib during an exam, EKG, smartwatch alert, or hospital visit.
Electrophysiology, often shortened to EP, is the area of cardiology focused on the heart’s electrical system. At Citrus Cardiology Consultants, PLLC, electrophysiology care may be recommended when a patient has an abnormal heart rhythm, symptoms that suggest an arrhythmia, or atrial fibrillation that requires a more specialized rhythm-management plan.
The goal of EP care is not simply to “stop AFib” in a general sense. It is to understand why the rhythm problem is happening, how often it occurs, how much it affects the patient, whether it increases stroke risk, and which treatment approach offers the best balance of safety, symptom relief, and long-term benefit.
What Is Electrophysiology?
Electrophysiology is a subspecialty of cardiology that studies and treats abnormal heart rhythms, also known as arrhythmias. The heart has its own electrical network. This system tells the upper and lower chambers when to beat, helping blood move efficiently through the heart and to the rest of the body.
When that electrical system becomes disorganized, too fast, too slow, or irregular, patients may experience symptoms — or may develop risks even without obvious symptoms. An electrophysiologist is a cardiologist with specialized training in diagnosing and treating heart rhythm disorders, including atrial fibrillation, atrial flutter, supraventricular tachycardia, ventricular arrhythmias, and slow heart rhythms that may require pacemaker therapy.
For atrial fibrillation, EP care is especially important because AFib is not the same in every patient. Some people have brief episodes that come and go. Others have persistent AFib that lasts longer or becomes more difficult to control. Some patients mainly need stroke prevention and rate control, while others may benefit from rhythm-control strategies such as cardioversion, antiarrhythmic medication, or catheter ablation.
Understanding Atrial Fibrillation
Atrial fibrillation occurs when the upper chambers of the heart, called the atria, beat in a rapid and disorganized way. Instead of contracting in a smooth rhythm, the atria quiver or fibrillate. This can cause an irregular heartbeat and may reduce how efficiently the heart moves blood.
AFib matters for two major reasons. First, it can cause symptoms that interfere with daily life, including palpitations, fatigue, shortness of breath, chest discomfort, dizziness, or reduced stamina. Second, AFib can increase the risk of stroke because blood may pool in the upper chambers and form clots. If a clot travels to the brain, it can cause a stroke.
For that reason, AFib treatment often has several goals: reduce stroke risk, control heart rate, restore or maintain normal rhythm when appropriate, relieve symptoms, and address underlying factors such as high blood pressure, sleep apnea, obesity, diabetes, thyroid disease, alcohol use, or other cardiovascular conditions.
How EP Helps Evaluate AFib
An EP evaluation begins with understanding the patient’s full clinical picture. This may include symptoms, frequency of episodes, prior EKG findings, heart monitor results, medications, medical history, family history, and other cardiac testing. A standard EKG may confirm AFib if the rhythm is present during the test, but because AFib can come and go, longer monitoring may be needed.
Holter monitors, event monitors, mobile cardiac telemetry, implantable loop recorders, echocardiograms, stress testing, and lab work may all be considered depending on the situation. The goal is to determine the type and burden of AFib, whether other rhythm problems are present, and whether there are structural or medical issues contributing to the arrhythmia.
This careful evaluation matters because the best treatment for one patient may not be the best treatment for another. A younger patient with highly symptomatic intermittent AFib may need a different strategy than an older patient with minimal symptoms but a higher stroke-risk profile.
EP Treatment Options for Atrial Fibrillation
EP treatment for AFib may include medication, procedures, lifestyle-focused risk reduction, or a combination of approaches. Treatment plans are individualized based on symptoms, stroke risk, heart function, other medical conditions, and patient preferences.
One common approach is rate control, which focuses on keeping the heart rate from becoming too fast while AFib is present. Another approach is rhythm control, which attempts to restore and maintain a normal rhythm. Rhythm-control options may include antiarrhythmic medications, electrical cardioversion, or catheter ablation.
Electrical cardioversion is a procedure that uses a controlled electrical shock to reset the heart rhythm. It can be effective for restoring normal rhythm, but AFib may return, especially if underlying triggers are not addressed.
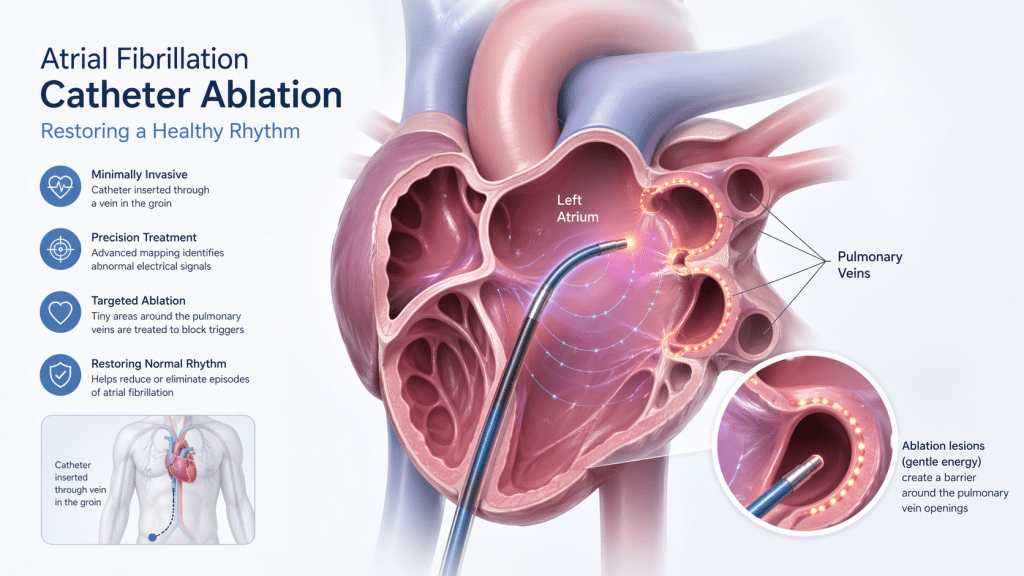
Catheter ablation is one of the most important EP procedures used to treat atrial fibrillation. During ablation, thin flexible tubes called catheters are guided through blood vessels to the heart. The electrophysiologist uses mapping technology to identify areas involved in the abnormal rhythm. Energy is then delivered to create small areas of scar tissue that block or isolate faulty electrical signals. For AFib, this often involves isolating the pulmonary veins, which are common sources of abnormal electrical triggers. The American Heart Association describes ablation as a procedure that targets tissue causing rapid or irregular heartbeats in order to help restore a more regular rhythm.
Different energy sources may be used in modern ablation, including radiofrequency energy, cryoablation, and newer approaches such as pulsed field ablation in selected settings. The specific method depends on the patient, the physician’s judgment, available technology, and the clinical situation.
Benefits and Limitations of AFib Ablation
For appropriately selected patients, AFib ablation may reduce episodes of atrial fibrillation, improve symptoms, reduce AFib-related hospital visits, and improve quality of life. However, it is not a guaranteed cure, and some patients may need more than one procedure. AFib can recur, particularly in the first weeks or months after ablation, and long-term success depends on several factors, including the type of AFib, heart structure, age, other medical conditions, and lifestyle risk factors. The NHLBI notes that ablation is not always successful and that AFib can recur after the procedure.
It is also important to understand that ablation does not automatically eliminate the need for blood thinners. Stroke-prevention decisions are usually based on a patient’s overall stroke risk, not simply whether the heartbeat feels normal after treatment.
As with any invasive procedure, catheter ablation has potential risks. These may include bleeding, infection, blood vessel injury, heart rhythm complications, damage to heart structures, blood clots, stroke, or other rare but serious complications. A careful EP consultation helps patients understand whether the potential benefits outweigh the risks in their specific case.
Why EP Expertise Matters
Atrial fibrillation can be simple to name but complex to manage. The rhythm itself is only one part of the decision. A thoughtful EP approach looks at the whole patient: symptoms, stroke risk, heart function, other conditions, medication tolerance, prior treatment response, and long-term goals.
Citrus Cardiology Consultants, PLLC has taken a leading role in this field by establishing the Citrus Cardiology Center for Heart Rhythm Management, a dedicated center staffed by physicians who are trained and experienced in electrophysiology. This gives patients with atrial fibrillation and other rhythm disorders access to specialized evaluation, advanced rhythm-focused care, and individualized treatment planning within the Citrus Cardiology network.
For patients, this level of expertise matters. AFib treatment may involve monitoring, medication, stroke-prevention strategies, cardioversion, catheter ablation, or a combination of approaches. Having physicians with focused electrophysiology training helps ensure that each option is considered carefully and that recommendations are based on the patient’s specific rhythm problem, health history, symptoms, and goals.
At Citrus Cardiology Consultants, PLLC, electrophysiology care is part of a comprehensive cardiovascular approach. Patients with AFib may benefit from coordinated evaluation, rhythm monitoring, medication management, procedural care when appropriate, and long-term follow-up designed to reduce risk and improve daily life.
Frequently Asked Questions About Electrophysiology and AFib
What does an electrophysiologist do?
An electrophysiologist is a cardiologist who specializes in the heart’s electrical system. They diagnose and treat abnormal heart rhythms such as atrial fibrillation, atrial flutter, SVT, and other arrhythmias.
Does every AFib patient need an EP procedure?
No. Some patients are managed with medication, monitoring, and risk-factor control. EP procedures such as ablation are considered based on symptoms, AFib pattern, medical history, and treatment goals.
What is catheter ablation for AFib?
Catheter ablation is a minimally invasive procedure that uses catheters to reach the heart and target areas responsible for abnormal electrical signals. The goal is to reduce or stop AFib episodes.
Is AFib ablation a cure?
Not always. Many patients have significant improvement, but AFib can return, and some patients need repeat treatment or ongoing medication.
Will I still need blood thinners after ablation?
Possibly. Blood thinner decisions are usually based on stroke risk factors such as age, blood pressure, diabetes, prior stroke, and other conditions, not only on whether AFib symptoms improve.
What symptoms should prompt an AFib evaluation?
Palpitations, racing heartbeat, fluttering, shortness of breath, dizziness, fainting, chest discomfort, or unexplained fatigue should be discussed with a medical provider.
When should I seek emergency care?
Call 911 or seek emergency care for chest pain, severe shortness of breath, fainting, symptoms of stroke, or a rapid heartbeat with severe weakness or distress.
📅 Last updated: