Coronary Angioplasty: Opening Blocked Heart Arteries and Restoring Blood Flow
When a coronary artery becomes narrowed or blocked, the heart muscle may not receive the oxygen-rich blood it needs to work properly. For many patients, this can lead to chest pressure, shortness of breath, fatigue, discomfort in the arm, jaw, neck, or back, or symptoms that appear during activity and improve with rest. In more urgent situations, a sudden blockage can contribute to a heart attack. Coronary angioplasty is one of the important procedures cardiologists may use to improve blood flow through a narrowed heart artery and help reduce symptoms related to coronary artery disease.
At Citrus Cardiology Consultants, PLLC, patients are evaluated carefully to determine whether coronary angioplasty is appropriate for their condition, symptoms, test results, and overall health. The goal is not simply to perform a procedure, but to choose the right treatment plan for the right patient at the right time.
What Is Coronary Angioplasty?
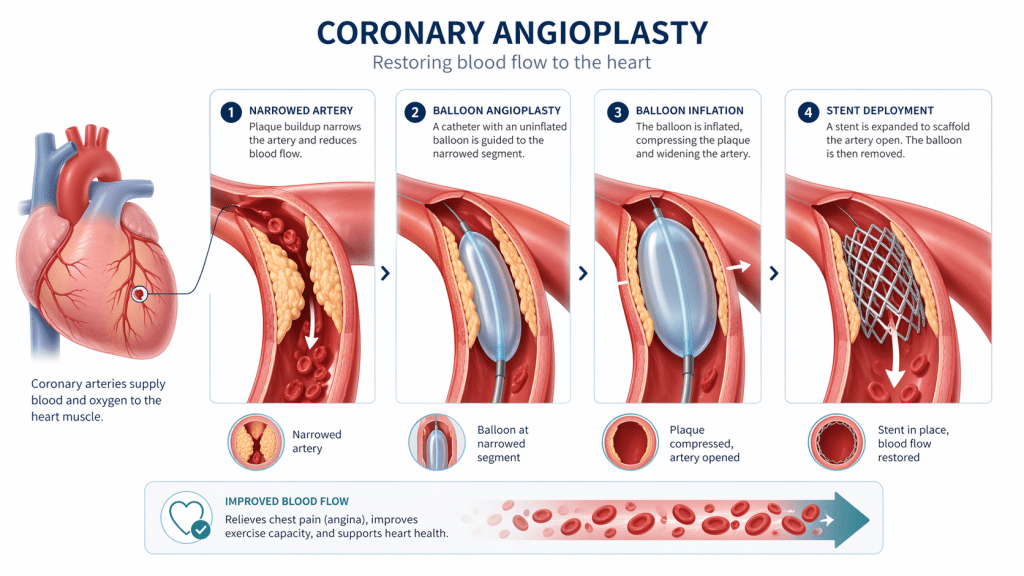
Coronary angioplasty, also called percutaneous coronary intervention or PCI, is a minimally invasive procedure used to open narrowed or blocked coronary arteries. These are the arteries that supply blood to the heart muscle. During angioplasty, a cardiologist guides a thin tube called a catheter through a blood vessel, usually from the wrist or groin, toward the affected artery in the heart. A small balloon at the tip of the catheter is then inflated at the narrowed area to press plaque against the artery wall and widen the passage for blood flow.
In many cases, a stent is placed during the procedure. A stent is a tiny mesh tube that remains inside the artery to help keep it open after the balloon is deflated and removed. Many modern stents are drug-eluting, meaning they slowly release medication designed to reduce the chance of the artery narrowing again.
Why Coronary Angioplasty May Be Recommended
Coronary angioplasty may be recommended when a patient has significant narrowing in one or more coronary arteries, especially if that narrowing is causing symptoms or limiting blood flow to the heart. It may be used to treat chest pain known as angina, improve blood flow after abnormal cardiac testing, or open an artery during certain types of heart attack.
Patients often wonder whether angioplasty “cures” heart disease. The answer is important: angioplasty can improve blood flow through a specific narrowed artery, but it does not remove the underlying tendency to develop plaque. Coronary artery disease is usually a long-term condition that also requires medical therapy, lifestyle changes, risk-factor control, and ongoing cardiology follow-up.
What Patients Can Expect During the Procedure
Coronary angioplasty is typically performed in a cardiac catheterization lab. Patients are usually awake but given medication to help them relax. The access area, commonly the wrist or groin, is numbed with local anesthesia. The cardiology team then inserts the catheter and uses imaging guidance to move it through the blood vessels to the heart.
Once the narrowed artery is reached, the balloon is inflated for a short period of time. Patients may feel brief chest pressure when the balloon is expanded because blood flow is temporarily reduced during that moment. If a stent is needed, it is expanded into place and left in the artery permanently to support the vessel wall. The catheter and balloon are then removed, and the access site is closed or bandaged.
The procedure time can vary depending on the number, location, and complexity of blockages. Some patients go home the same day, while others stay overnight for monitoring, especially if the angioplasty was performed during a heart attack or if additional medical concerns are present.
Benefits and Limitations
For properly selected patients, coronary angioplasty can provide meaningful benefits. It may relieve angina, improve exercise tolerance, restore blood flow through a narrowed artery, and reduce damage to the heart muscle when performed urgently during a heart attack. A stent can help keep the artery open and support more reliable blood flow.
However, angioplasty is not the best choice for every patient. Some blockages may be better managed with medication, while others may require coronary artery bypass surgery. The decision depends on factors such as the number of narrowed arteries, the location of the blockage, heart function, diabetes status, kidney function, symptoms, and overall risk profile.
There are also potential risks, as with any medical procedure. These can include bleeding or bruising at the catheter site, artery injury, blood clots, allergic reaction to contrast dye, abnormal heart rhythm, kidney strain from contrast dye, restenosis, heart attack, stroke, or the need for emergency surgery, though serious complications are uncommon in appropriately selected patients.
Recovery After Coronary Angioplasty
After the procedure, patients are monitored closely. The care team checks heart rhythm, blood pressure, oxygen levels, and the catheter access site. If the catheter was inserted through the groin, patients may need to lie flat for several hours to reduce the risk of bleeding. If the wrist was used, recovery may involve a compression band and careful monitoring of the hand and arm.
Before going home, patients receive specific instructions about activity, medications, wound care, and follow-up appointments. Most patients are advised to avoid heavy lifting or strenuous activity for a short period. It is also common to be prescribed antiplatelet medication, which helps reduce the risk of blood clots forming inside the stent. It is very important not to stop these medications unless instructed by the cardiology team. Patients with a stent remain at risk for future heart problems, so long-term care remains essential.
A Procedure Is Only One Part of Heart Care
Coronary angioplasty can be an important part of treating coronary artery disease, but it works best as part of a broader heart-care plan. That plan may include cholesterol management, blood pressure control, diabetes care, smoking cessation, nutrition guidance, exercise recommendations, cardiac rehabilitation, and regular cardiology follow-up.
At Citrus Cardiology Consultants, PLLC, the emphasis is on comprehensive cardiovascular care. Patients receive individualized evaluation and guidance so that treatment decisions are based on their symptoms, test results, risk factors, and long-term health goals. If you have been told you may have a blocked heart artery, or if you are experiencing symptoms that could be related to reduced blood flow to the heart, a cardiology evaluation can help determine the safest and most effective next step.
Frequently Asked Questions About Coronary Angioplasty
Is coronary angioplasty the same as heart surgery?
No. Coronary angioplasty is minimally invasive and does not involve opening the chest. It is performed using catheters inserted through a blood vessel, usually in the wrist or groin.
Will I be asleep during the procedure?
Most patients are awake but relaxed with medication. The access area is numbed, and the care team monitors you closely throughout the procedure.
Does angioplasty hurt?
Patients may feel pressure at the access site or brief chest pressure when the balloon is inflated, but significant pain is not expected. Tell your care team immediately if you feel discomfort.
Is a stent always placed?
Not always, but stents are commonly used during coronary angioplasty to help keep the artery open. Your cardiologist will determine whether a stent is appropriate based on the artery and blockage.
How long does recovery take?
Recovery varies. Many patients return to light activity within a few days, but instructions depend on the access site, the reason for the procedure, and the patient’s overall condition.
Are there alternatives to angioplasty?
Yes. Depending on the situation, alternatives may include medication management, lifestyle changes, cardiac rehabilitation, or coronary artery bypass surgery.
When should I seek urgent medical care after angioplasty?
Call 911 or seek emergency care for chest pain, severe shortness of breath, fainting, signs of stroke, uncontrolled bleeding, or sudden swelling or pain at the catheter site.
📅 Last updated: